La plantilla oficial no se publicará hasta el 13 de febrero
Preguntas y las posibles respuestas del examen MIR de 2018.
#MIR #MIR2018
La escuela profesional Ceisal ha distribuido la mañana de este domingo cuatro copias de las cuatro versiones de la prueba:
versión 1
versión 2
versión 3
versión 4
Listados de respuestas
versión 1
versión 2
versión 3
versión 4, en todas sus versiones corregidos por sus profesores.35 imágenes de alta calidad -consulte aquí el cuaderno de imágenes-.
Como ya adelantó Redacción Médica, entre las 225 preguntas y las 10 de reserva se han expuesto un total de 35 imágenes de alta calidad, para responder sobre las mismas -consulte aquí el cuaderno de imágenes-. Sigue de este modo cogiendo peso la exposición de fotografías, como ya sucedió en convactorias anteriores. Precisamente, las imagenes de este año han marcado parte de la dificultad del examen. En opinión de algunos de los aspirantes consultados por este medio, se ha tratado de un examen con una dificultad alta, aunque "asequible para quien haya venido preparado". A pesar de que estos resultados preliminares permiten hacerse una idea sobre qué puesto se ha alcanzado en la actual convocatoria MIR, estas respuestas no tienen validez legal. Las certezas comenzarán para los aspirantes a partir del momento en el que Sanidad publique los resultados provisionales.La plantilla provisional de respuestas correctas se publicará el próximo día 13 de febrero, y el plazo para presentar impugnaciones contra la misma será del 14 al 16 de febrero. El día 28 de febrero se reunirá la Comisión Calificadora para resolver las impugnaciones y publicar la plantilla de respuestas correctas definitiva. Con la misma el Ministerio de Sanidad corregirá los exámenes, y el día 6 de marzo, publicará los resultados provisionales de la prueba, incluido el baremo académico y el número de orden provisional. Hasta esa fecha no se sabrá con certeza el futuro de cada uno de los aspirantes presentados a las pruebas de Formación Sanitaria Especializada.

Domingo, 11 de febrero de 2018, a las 20:20
Neurología y Cardiología han sido los dos temas que más cuestiones han aglutinado con 19 preguntas

Domingo, 11 de febrero de 2018, a las 13:50
En muchos casos, la nota del expediente académico será el punto diferenciador entre conseguir o no plaza

Domingo, 11 de febrero de 2018, a las 12:30
La cuestión sobre el nivel de ruido de una aeronave copa las críticas en redes sociales

Domingo, 11 de febrero de 2018, a las 11:00
Una pregunta sobre homeopatía se cuela entre las 225 cuestiones del examen FIR 2018

Domingo, 11 de febrero de 2018, a las 10:50
La plantilla oficial no se publicará hasta el 13 de febrero

Domingo, 11 de febrero de 2018, a las 10:20
La dificultad del examen marca el día después de la prueba, con valoraciones que van del pesimismo al humor

Domingo, 11 de febrero de 2018, a las 09:00
El calendario para conocer los resultados definitivos se prolonga hasta abril

Sábado, 10 de febrero de 2018, a las 23:40
Los aspirantes de Enfermería creen que el examen no se corresponde con la realidad de las asignaturas

Sábado, 10 de febrero de 2018, a las 22:50
El examen de este año ha seguido la tónica de los anteriores y no ha presentado grandes sorpresas

Sábado, 10 de febrero de 2018, a las 21:00
Redacción Médica le toma el pulso a la dificultad de la prueba a través de la opinión de los propios candidatos

Sábado, 10 de febrero de 2018, a las 17:40
Más de 40 centros, casi mil interventores y 532 mesas de examen sientan hoy a más de 33.000 aspirantes a la FSE

Sábado, 10 de febrero de 2018, a las 16:00
Miles de candidatos se juegan su futuro en las pruebas de FSE y, como cada año, los rituales son los mismos

Viernes, 09 de febrero de 2018, a las 16:10
La prueba dará comienzo a las 16:00 horas y tendrá una duración de cinco horas

Viernes, 09 de febrero de 2018, a las 13:40
Miguel Sáez Alegre, tutor de CTO, da las claves que siguió él antes de someterse a la prueba que le convirtió en MIR

Viernes, 09 de febrero de 2018, a las 09:10
Falta poco para el examen MIR. ¿Eres capaz de sacar plaza? Atrévete con este cuestionario de preguntas que podrían salir

Viernes, 09 de febrero de 2018, a las 09:10
La dietista-nutricionista, Rocío Maraver, da varios consejos para llegar a las pruebas de FSE llenos de energía

Jueves, 08 de febrero de 2018, a las 18:40
El e-mail adjunta un documento referido a la elección de plaza MIR por vía telemática

Jueves, 08 de febrero de 2018, a las 16:00
La presencia femenina será del 69% frente al 32% de hombres en la convocatoria de Formación Sanitaria Especializada

Jueves, 08 de febrero de 2018, a las 13:00
Así lo ha confirmado el Ministerio de Sanidad en su nota de prensa previa a la convocatoria oficial

Jueves, 08 de febrero de 2018, a las 12:40
Rubén Martín, tutor de CTO, ejemplifica esta situación con un ejemplo drástico pero práctico para el día de la prueba

Martes, 06 de febrero de 2018, a las 13:00
Chelu Martín, creador de MirMeApp, muestra cuales son las cuestiones en las que siempre caen los admitidos al MIR

Martes, 06 de febrero de 2018, a las 12:30
Cinco preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Lunes, 05 de febrero de 2018, a las 14:10
El examen ha congregado en Madrid a más de 2.000 estudiantes de la academía

Lunes, 05 de febrero de 2018, a las 09:15
Falta poco para el examen MIR. ¿Eres capaz de sacar plaza? Atrévete con este cuestionario de preguntas que podrían salir

Sábado, 03 de febrero de 2018, a las 18:00
Grupo CTO celebra este sábado un simulacro MIR que dará cita a miles de aspirantes, una semana antes de la gran cita

Viernes, 02 de febrero de 2018, a las 12:00
Una sola lata contienen un equivalente a 13 terrones de azúcar, lo que puede derivar en problemas de obesidad

Viernes, 02 de febrero de 2018, a las 09:10
Imane Jeidane realizará el examen FIR como extracomunitaria y peleará por una de las 7 plazas disponibles

Jueves, 01 de febrero de 2018, a las 13:00
Este sistema va dirigido a los candidatos cuyo documento de identidad no les permite obtener un certificado electrónico

Jueves, 01 de febrero de 2018, a las 10:00
Falta poco para el examen MIR. ¿Eres capaz de sacar plaza? Atrévete con este cuestionario de preguntas que podrían salir

Miércoles, 31 de enero de 2018, a las 17:50
Las voces que lograron convertirse en los primeros en elegir especialidad MIR coinciden: Disciplina e ilusión

Martes, 30 de enero de 2018, a las 12:00
A falta de dos semanas para celebrar la prueba, los 14.450 apuran las horas repasando los temas principales del MIR

Martes, 30 de enero de 2018, a las 10:25
El coordinador de MIR de Semergen destaca la sorpresa de los residentes con la cantidad de pruebas que pueden realizar

Martes, 30 de enero de 2018, a las 09:20
Voro Dasí, candidato al PIR, ha aplicado lo aprendido durante la carrera en su escueto proceso de preparación

Domingo, 28 de enero de 2018, a las 11:20
Falta poco para el examen MIR. ¿Eres capaz de sacar plaza? Atrévete con este cuestionario de preguntas que podrían salir

Sábado, 27 de enero de 2018, a las 20:00
Estefanía ya es médica de Familia, pero comenta que la experiencia profesional no hace más fácil la prueba

Viernes, 26 de enero de 2018, a las 09:10
Isabel Morales, candidata al FIR, cuenta con humor como ha sido su proceso de estudio durante estas navidades

Viernes, 26 de enero de 2018, a las 09:05
Los datos del Ministerio de Sanidad vislumbran que la convocatoria de 2017 presentó la puntuación más alta

Jueves, 25 de enero de 2018, a las 12:30
La sexóloga Raquel Graña detalla las ventajas de mantener una vida sexual saludable

Jueves, 25 de enero de 2018, a las 09:20
Seis preguntas para ponerte a prueba a pocas semanas de la gran cita de la Formación Sanitaria Especializada

Jueves, 25 de enero de 2018, a las 09:05
Alberto dedica más de 10 horas a preparar el examen MIR y solo piensa en volver a recuperar su tiempo libre

Miércoles, 24 de enero de 2018, a las 12:50
La reducción de plazas en Formación Sanitaria Especializada se ha ido recuperando paulatinamente en los últimos años

Martes, 23 de enero de 2018, a las 16:50
Una tuitera comparte los 16 dilemas que se les pasan por la cabeza a los aspirantes de la convocatoria de febrero

Martes, 23 de enero de 2018, a las 12:50
Según datos del Ministerio de Educación, los estudiantes saltan directamente a la preparación del MIR

Lunes, 22 de enero de 2018, a las 12:00
La asignatura de Digestivo fue la que más preguntas recopiló

Domingo, 21 de enero de 2018, a las 10:00
Seis preguntas para ponerte a prueba a pocas semanas de la gran cita de la Formación Sanitaria Especializada

Sábado, 20 de enero de 2018, a las 20:00
A María se le resistieron dos asignaturas y acabó la carrera "muy cansada mentalmente"

Sábado, 20 de enero de 2018, a las 16:00
La demanda total para estudiar Medicina asciende hasta las 46.408 candidaturas

Sábado, 20 de enero de 2018, a las 10:30
Un estudiante se graba durante un día entero para ver la evolución que experimenta durante su jornada de estudio al MIR

Martes, 16 de enero de 2018, a las 11:30
La Dirección General de Ordenación Profesional ultima los preparativos de la prueba

Martes, 16 de enero de 2018, a las 10:40
El Ministerio de Sanidad ha nombrado las comisiones calificadoras de las pruebas para las plazas de formación sanitaria

Lunes, 15 de enero de 2018, a las 17:20
Los médicos de Familia creen que falta concienciación sobre la especialidad de Atención Primaria en la universidad

Domingo, 14 de enero de 2018, a las 13:15
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Sábado, 13 de enero de 2018, a las 20:00
Cristina quiere hacer Cardiología en Madrid y afronta el examen con tranquilidad: “La autoconfianza da puntos”

Viernes, 12 de enero de 2018, a las 09:10
Seis preguntas para ponerte a prueba a falta de un mes de la gran cita de la Formación Sanitaria Especializada

Jueves, 11 de enero de 2018, a las 14:00
Por cada siete admitidos al MIR de origen extracomunitario, solo uno conseguirá una plaza

Jueves, 11 de enero de 2018, a las 09:10
Los 14.450 candidatos admitidos a la prueba se repartirán por todo el territorio español para lograr su objetivo

Martes, 09 de enero de 2018, a las 11:40
La lista definitiva de aspirantes se reduce respecto a 2017

Martes, 09 de enero de 2018, a las 11:30
El próximo 10 de febrero cada 31 candidatos aspirarán a una de las 135 plazas disponibles

Martes, 09 de enero de 2018, a las 11:30
Estas cifras suponen un aumento de 54 aspirantes con respecto a las listas provisionales de noviembre

Martes, 09 de enero de 2018, a las 10:20
Con esta ampliación, el número de aspirantes por cada plaza asciende a 11,14

Martes, 09 de enero de 2018, a las 09:30
La actual convocatoria tendrá 2,21 aspirantes por cada plaza ofertada

Lunes, 08 de enero de 2018, a las 18:30
Las candidaturas rechazadas suman un total de 537

Domingo, 07 de enero de 2018, a las 12:00
Claudio Rivadulla, tutor de Grupo CTO, aporta algunos trucos para superar las más de cinco horas que dura la prueba

Viernes, 05 de enero de 2018, a las 09:30
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Miércoles, 03 de enero de 2018, a las 09:30
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Martes, 02 de enero de 2018, a las 09:05
Antonio Martín, profesor MIR de CTO, revela las asignaturas con más opciones de ser preguntadas en la prueba MIR

Sábado, 30 de diciembre de 2017, a las 14:00
Catuxa Argibay explica que es fundamental mantener la constancia y la serenida durante la preparación del examen EIR

Jueves, 28 de diciembre de 2017, a las 12:50
El Consejo General de la Psicología de España exige acabar con el acceso de otras titulaciones al examen PIR
Domingo, 24 de diciembre de 2017, a las 10:30
Los aspirantes tienen a su disposición recopilaciones de la misma duración que los exámenes

Sábado, 23 de diciembre de 2017, a las 14:50
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Sábado, 23 de diciembre de 2017, a las 10:20
Sin chocolatinas y con mucho repaso, miles de estudiantes al examen MIR entran en su recta final y deben prepararse

Domingo, 17 de diciembre de 2017, a las 10:35
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Sábado, 16 de diciembre de 2017, a las 10:50
Un youtuber se encarga de recetar desde su propia experiencia varios consejos para ayudar al candidato MIR

Viernes, 15 de diciembre de 2017, a las 09:15
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Domingo, 10 de diciembre de 2017, a las 10:20
Jorge García, subdirector de Grupo CTO, explica las claves para triunfar en la prueba MIR

Sábado, 09 de diciembre de 2017, a las 12:40
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Martes, 05 de diciembre de 2017, a las 09:10
Seis preguntas para ponerte a prueba a pocos meses antes de la gran cita de la Formación Sanitaria Especializada

Viernes, 01 de diciembre de 2017, a las 12:50
El plazo de diez días fijado por el Ministerio de Sanidad hace referencia a días laborables, y no naturales

Viernes, 01 de diciembre de 2017, a las 09:20
A escasas horas para cerrar el plazo de reclamación, el Ministerio de Sanidad sigue revisando solicitudes

Jueves, 30 de noviembre de 2017, a las 09:20
La muestra enviada por el Ministerio a la empresa encargada de su impresión marca un total de 235 respuestas

Viernes, 24 de noviembre de 2017, a las 09:30
Daniel, candidato por segunda vez al examen MIR, evidencia las carencias del modelo de formación sanitaria

Jueves, 23 de noviembre de 2017, a las 11:30
El Consejo General de la Enfermería denuncia esta situación y exige más plazas para especialistas

Jueves, 23 de noviembre de 2017, a las 10:10
Eneko Armendáriz, representante de los estudiante de Enfermería, critica el ratio de plaza del EIR por candidato

Miércoles, 22 de noviembre de 2017, a las 12:30
Las solicitudes afectadas por el cupo suponen el 16% del total del MIR

Martes, 21 de noviembre de 2017, a las 13:20
En cifras totales, el ratio provisional de plaza en la convocatoria de Formación Sanitaria es de 3,4 por participante

Martes, 21 de noviembre de 2017, a las 12:20
Barcelona, Oviedo y Valencia completan el grupo de sedes con más de 1.000 candidatos

Martes, 21 de noviembre de 2017, a las 11:30
El plazo para reclamar durará diez días y comenzará a contar a partir de este miércoles

Martes, 21 de noviembre de 2017, a las 10:50
En total, el número de aspirantes que se presentan a este examen ha sido de 4.228, 246 más que en la edición anterior

Martes, 21 de noviembre de 2017, a las 10:40
La tasa de rechazados por el Ministerio de Sanidad alcanza el 6,65% del total de inscritos

Martes, 21 de noviembre de 2017, a las 10:40
El número de no admitidos provisionales no llega a la centena y se sitúa en las 71 candidaturas que deberán de reclamar

Martes, 21 de noviembre de 2017, a las 10:30
Este año 1.233 candidatos provisionales optarán a 245 plazas, una plaza por cada cinco aspirantes

Martes, 21 de noviembre de 2017, a las 00:20
El número de solicitudes no admitidas ronda las 1.565

Sábado, 18 de noviembre de 2017, a las 20:00
La Revista de Redacción Médica habla con residentes de diferentes especialidades para conocer sus perspectivas laborales

Sábado, 18 de noviembre de 2017, a las 12:20
Prosegur Servicios gana el contrato encargado de proteger los exámenes de las pruebas de Formación Sanitaria

Viernes, 17 de noviembre de 2017, a las 10:50
El Ministerio ha modificado el calendario oficial de la convocatoria de admitidos provisionales hasta en dos ocasiones

Jueves, 16 de noviembre de 2017, a las 12:20
Finalmente, las listas provisionales se podrán consultar el próximo martes 21 de noviembre

Lunes, 13 de noviembre de 2017, a las 12:30
Jorge Martínez quiere que sus consejos ayuden a los futuros candidatos del examen de 2018

Lunes, 13 de noviembre de 2017, a las 09:30
Melilla, Ceuta y Castilla-La Mancha son las tres regiones con menos residentes por cada 100.000 habitantes

Miércoles, 01 de noviembre de 2017, a las 16:20
La inestabilidad social y política despierta la incertidumbre de los residentes MIR sobre su futuro en Cataluña

Martes, 31 de octubre de 2017, a las 19:00
La sobrecarga laboral o las excesivas horas de guardia son algunos de las carencias que exigen resolver

Lunes, 30 de octubre de 2017, a las 11:20
En total, la horquilla de interventores que maneja el ministerio de Sanidad para supervisar los exámenes es de 428-483

Viernes, 27 de octubre de 2017, a las 08:00
El plazo para poder solicitar ser interventor se inicia desde el día 25 de octubre hasta el próximo 22 de noviembre

Sábado, 07 de octubre de 2017, a las 10:00
Su oferta se distribuye entre 81 hospitales, entre los que se encuentran los más importantes del país

Jueves, 05 de octubre de 2017, a las 17:30
La representante del CEEM en el congreso de Educación Médica, Sara Vargas, ha rechazado la apertura de nuevas facultades

Jueves, 05 de octubre de 2017, a las 14:20
En total, la previsión realizada por el Ministerio de Sanidad es de 14.450 aspirantes médicos

Lunes, 02 de octubre de 2017, a las 13:10
Un estudio revela la importancia que ha ido ganando esta especialidad, año tras año

Lunes, 02 de octubre de 2017, a las 12:00
El CEEM pide un compromiso por escrito al ministerio que dirige Dolors Montserrat

Jueves, 28 de septiembre de 2017, a las 19:20
Carlos Moreno, director general de Ordenación Profesional, da pistas sobre el nuevo modelo de troncalidad

Jueves, 28 de septiembre de 2017, a las 09:20
El plazo de presentación de instancias finaliza este jueves 28 de septiembre

Miércoles, 20 de septiembre de 2017, a las 09:20
Cataluña es la comunidad que más plazas gana, pero es Madrid la que sigue acaparando la mayor oferta disponible

Martes, 19 de septiembre de 2017, a las 11:10
El Modelo 790 ya está disponible para proceder a la solicitud de acceso a las pruebas

Lunes, 18 de septiembre de 2017, a las 16:50
La mayor oferta de plazas se da en el Gregorio Marañón y el 12 de Octubre de Madrid, ambos con 99 puestos

Lunes, 18 de septiembre de 2017, a las 14:40
Sanidad oferta 13 vacantes más para este colectivo, hasta alcanzar un total de 456 para la convocatoria de 2018

Domingo, 17 de septiembre de 2017, a las 10:50
La convocatoria de 2017 trae consigo varias novedades que se suman a las ya incluidas en 2016

Sábado, 16 de septiembre de 2017, a las 11:50
Esta medida es posible gracias a la Ley 39/2015, de 1 de octubre, que entra en vigor en esta convocatoria

Viernes, 15 de septiembre de 2017, a las 15:30
La oferta de plazas total para estas seis titulaciones son de 1.544 plazas

Viernes, 15 de septiembre de 2017, a las 13:40
Este viernes Sanidad ha emitido un escrito aclaratorio para todos aquellos que se presentan al examen

Viernes, 15 de septiembre de 2017, a las 11:50
Cirugía Cardiovascular es la mayor damnificada de esta convocatoria

Viernes, 15 de septiembre de 2017, a las 11:20
El incremento total de plazas en el sector público se cuantifica en 185

Viernes, 15 de septiembre de 2017, a las 09:50
Medicina de Familia acapara 1.810 de las 6.513 plazas ofertadas

Jueves, 14 de septiembre de 2017, a las 16:20
Como ya adelantó Redacción Médica, la fecha de los exámenes de Formación Especializada será el próximo 10 de febrero

Sábado, 09 de septiembre de 2017, a las 10:00
Aunque el incremento global ha sido de 285 plazas, existen dos comunidades autónomas que han perdido plazas

Domingo, 03 de septiembre de 2017, a las 19:30
Ambas comunidades suman un total de 2.770 plazas destinadas a Formación Sanitaria Especializada

Sábado, 26 de agosto de 2017, a las 17:10
El Ministerio de Sanidad todavía tiene que oficializarla mediante su publicación en el BOE
Jueves, 03 de agosto de 2017, a las 16:10
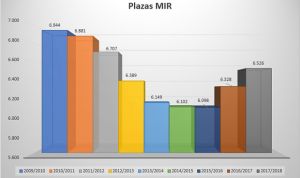
El Ministerio de Sanidad ha creado 428 plazas nuevas, revirtiendo en más de la mitad el recorte de residentes
Miércoles, 02 de agosto de 2017, a las 09:50
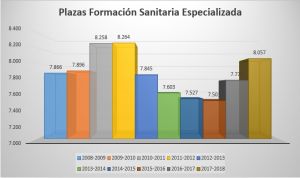
El crecimiento de 267 plazas de esta convocatoria permite que la oferta de este año supere la barrera de los 8.000

Martes, 01 de agosto de 2017, a las 12:00
El cupo del 4% limitará el acceso de facultativos foráneos, estableciéndolo en un total de 261 plazas

Lunes, 31 de julio de 2017, a las 18:20
El Ministerio de Sanidad publica los datos correspondientes a la mediana del número de orden de la última convocatoria

Viernes, 28 de julio de 2017, a las 10:10
Aunque Sara Vargas, vicepresidenta de Asuntos Externos de CEEM, reconoce que es "un primer paso" positivo

Jueves, 27 de julio de 2017, a las 14:00
La cifra de médicos esta convocatoria se incrementa un 3,2 por ciento con respecto a la anterior

Jueves, 27 de julio de 2017, a las 11:30
Varios tutores de diferentes hospitales universitarios explican estas situaciones

Miércoles, 26 de julio de 2017, a las 18:40
Andalucía duplica el crecimiento medio estatal con un 7,47% y 1.224 plazas





















































































































































