 |
Vacuum spine boards: Transport devices of the future |
Dr. Ramon Reyes, MD
Vacuum spine boards: Transport devices of the future
They immobilize as well as backboards, are more comfortable, and reduce tissue interface pressures
February 27, 2014
The Research Review
By Kenny Navarro
An unstable spinal column with an undamaged spinal cord probably represents one of the greatest management challenges for emergency medical personnel.
In 2010, the National Spinal Cord Injury Statistical Center[1] reported approximately 12,000 new cases of spinal cord injury in the United States each year. Injuries to the spinal cord can produce catastrophic consequences — usually immediately following the traumatic event, although some effects do not fully develop until sometime after. In some patients, damage to the boney vertebrae may occur but the cord itself may be intact.
Rescue devices such as long backboards, short backboards, and extrication vests offer restrictions to movement, but they do not immobilize[2].
Advanced care providers have long recognized the potential harm that accompanies the use of rigid spinal immobilization, especially if prolonged.
Rescue work involves movement, as paramedics and EMTs must relocate the patient from hostile to more stable environments. Every device applied in the field only fastens externally to the patient; the skin and muscle will continue to slide across the skeletal frame and produce bone movement. Additional movement occurs during transport as the patient’s body is subject to the laws of physics and inertia.[3]
The spine board was developed as an extrication tool,[4] for EMS to use in conjunction with a cervical collar and restraining straps to prevent secondary spinal cord injury resulting from patient movement to the hospital. In many areas, this procedure has remained a standard of care for almost half a century, despite the lack of convincing evidence that the procedure improves patient outcome. [5]
Rigid spine boards
Bauer and Kowalski[6] demonstrated that immobilization on a long spine board resulted in significant reductions in forced vital capacity (volume of air that can be forced from the lungs after taking the deepest inhalation possible), forced expiratory volume (maximum volume of air that can be forcibly exhaled in one second), and forced expiratory flow (average airflow over specific portions of the spirometry curve) among healthy non-smoking males. These reductions, when coupled with airway or thoracic injuries, or in patients with a history of respiratory pathology, may significantly reduce the ability for adequate self-ventilation.
Researchers in North Carolina found similar reductions in pulmonary function testing associated with immobilization on a long spine board in children ages 6 to 15.[7]
Immobilization on a rigid backboard altered subsequent physical examination findings in about 20 percent of healthy volunteers by inducing cervical and lumbar midline point tenderness where none previously existed[5]. This could result in unnecessary and expensive testing when the patient arrives in the emergency department.
Research also demonstrates that immobilization on a rigid spine board can result in the development of pressure ulcers. Pressure ulcers develop over bony prominences in individuals that are immobilized on hard surfaces. The weight of the body and the unforgiving nature of the surface impair blood flow to the area, resulting in localized ischemia, cellular death and tissue necrosis.
Increasing the duration of immobilization or the magnitude of the applied pressure will increase the rate of pressure ulcer formation[8]. A study of patients with spinal cord injury found that all in-patients who developed skin ulcerations recalled no attempt to move or rotate them off the backboard within the first two hours after injury to relieve the pressure[9].
In contrast, all patients who did not develop ulcerations had the pressure relieved within the first two hours by someone who rotated their body off the spine board.
Researchers in New Orleans demonstrated a direct relationship between the duration spent on a spine board and the development of pressure ulcers within the first eight days of hospitalization[10]. As many as 31 percent of trauma patients will develop pressure ulcers as the result of immobilization on a backboard[11].[12]
Berg[13] (et al) found that immobilization for periods as short as 30 minutes can produce significant reductions in localized tissue oxygenation in healthy patients. Lerner and Moscoti[12] found that trauma patients spend an average of 64 minutes on a backboard including the time spent in the field. However, if radiographs were required for spinal injury clearance and backboard removal, total backboard time exceed three hours.
Cooney, Wallus, Asaly, and Wojcik[14] found the total time spent immobilized on a backboard can exceed seven hours when EMS first transports patients to a tertiary center and then transfers the patient to a Level 1 trauma center.
Vacuum spine boards
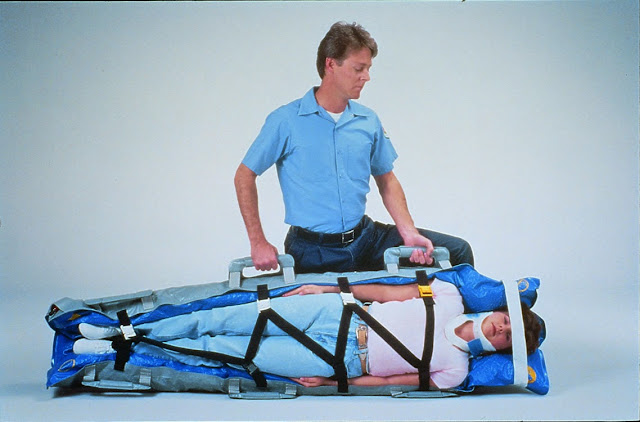
In an attempt to provide a more comfortable method for immobilizing the spine for transport to the emergency department, many EMS agencies are using a vacuum type splint device. Vacuum splints are flexible, waterproof shells filled with polystyrene beads similar to a very large beanbag.
Early in the application process, the splint is soft and malleable. Rescuers can push the beads into the recesses and voids between a patient and the splint. However after withdrawing the air, the splint conforms to the shape of the patient and becomes rigid.
In a side by side comparison with a rigid backboard, the vacuum splint device was judged more comfortable by the patient, was faster for rescuers to apply, and resulted in less body movement in the event the patient required tilting[15]. Healthy volunteers reported significantly less pain at 30 and 60 minutes when immobilized on a vacuum rather than a rigid spine board[16].
Pressure of about 35 mm Hg applied to the surface of the skin will significantly reduce blood flow through a capillary bed[17]. Interface pressures on good to high quality hospital mattresses vary between 30 and 60 mm Hg[18].
Researchers using pressure-mapping sensors on 20 healthy volunteers demonstrated that rigid spine boards produce the highest tissue interface pressures at the patient’s scapulae, sacrum, and heels when compared to the use of a standard, soft overlay mattress or a vacuum mattress[4].
The volunteers also rated the rigid spine board as the least comfortable device. This is consistent with a study by Lovell and Evans that demonstrated tissue interface pressures as high as 147 mm Hg with a rigid spine board, 115 mm Hg when the board was padded, but 37 mm Hg with a vacuum mattress[19].
The U.S. Army Institute of Surgical Research[20] has designated the vacuum spine board to be the immobilization method of choice during transport of patients suffering from potentially unstable thoracolumbar fractures. Unfortunately, military researchers could not demonstrate a significant reduction in pressure ulceration development associated with vacuum spine board use compared to historical controls using rigid spine boards[21].
However, more patients in the vacuum spine board group required endotracheal intubation, and thus were motionless for longer periods of time. There are anecdotal reports of awake and oriented patients becoming claustrophobic during prolonged transport while immobilized in a vacuum spine board.
Nonetheless, vacuum spine boards appear to provide a very promising alternative to the rigid spine boards historically used in EMS. These devices immobilize as well as backboards, are more comfortable for the patient, and reduce tissue interface pressures, which may reduce the development of pressure ulcerations resulting from the immobilization procedure itself.
 |
Vacuum spine boards: Transport devices of the future |
References
1. National Spinal Cord Injury Statistical Center (NSCISC). (2010). Spinal cord injury. Facts and figures at a glance. Retrieved from https://www.nscisc.uab.edu/
2. Shafer, J. S., & Naunheim, R. S. (2009). Cervical spine motion during extrication: A pilot study. Western Journal of Emergency Medicine, 10(2), 74-78.
3. Perry, S. D., McLellan, B., McIlroy, W. E., Maki, B. E., Schwartz, M., & Fernie, G. R. (1999). The efficacy of head immobilization techniques during simulated vehicle motion. Spine, 24(17), 1839–1844.
4. Keller, B. P., Lubbert, P. H., Keller, E., & Leenen, L. P. (2005). Tissue-interface pressures on three different support-surfaces for trauma patients. Injury, 36(8), 946-948.
5. March, J. A., Ausband, S. C., & Brown, L. H. (2002). Changes in physical examination caused by use of spinal immobilization. Prehospital Emergency Care, 6(4), 421-424.
6. Bauer, D., & Kowalski, R. (1988). Effect of spinal immobilization devices on pulmonary function in the healthy nonsmoking man. Annals of Emergency Medicine, 17(9), 915-918. doi:10.1016/S0196-0644(88)80671-1
7. Schafermeyer, R. W., Ribbeck, B. M., Gaskins, J., Thomason, S., Harlan, M., & Attkisson, A. (1991). Respiratory effects of spinal immobilization in children. Annals of Emergency Medicine, 20(9), 1017-1019. doi:10.1016/S0196-0644(05)82983-X
8. Vickery, D. (2001). The use of the spinal board after the pre-hospital phase of trauma management. Emergency Medicine Journal, 18(1), 51-54. doi:10.1136/emj.18.1.51
9. Linares, H. A., Mawson, A. R., Suarez, E., & Biundo, J. J. (1987). Association between pressure sores and immobilization in the immediate postinjury period. Orthopedics, 10(4), 571–573.
10. Mawson, A. R., Biundo, J. J. Jr., Neville, P., Linares, H. A., Winchester, Y., & Lopez, A. (1988). Risk factors for early occurring pressure ulcers following spinal cord injury. American Journal of Physical Medicine and Rehabilitation, 67(3), 123-127.
11. Baldwin, K. M., & Ziegler, S. M. (1998). Pressure ulcer risk following critical traumatic injury. Advances in Wound Care, 11(4), 168-173.
12. Watts, D., Abrahams, E., MacMillan, C., Sanat, J., Silver, R., Van Gorder, S., Waller, M., & York, D. (1998). Insult after injury: Pressure ulcers in trauma patients. Orthopaedic Nursing, 17(40), 84-91.
13. Berg, G., Nyberg, S., Harrison, P., Baumchen, J., Gurss, E., & Hennes, E. (2010). Near-infrared spectroscopy measurement of sacral tissue oxygen saturation in healthy volunteers immobilized on rigid spine boards. Prehospital Emergency Care, 14(4), 419-424. doi:10.3109/10903127.2010.493988
14. Cooney, D. R., Wallus, H., Asaly, M., & Wojcik, S. (2013). Backboard time for patients receiving spinal immobilization by emergency medical services. International Journal of Emergency Medicine, 6(1), 17. doi:10.1186/1865-1380-6-17
15. Johnson, D. R., Hauswald, M., & Stockhoff, C. (1996). Comparison of a vacuum splint device to a rigid backboard for spinal immobilization. American Journal of Emergency Medicine, 14(4), 369-372. doi:10.1016/S0735-6757(96)90051-0
16. Cross, D. A., & Baskerville, J. (2001). Comparison of perceived pain with different immobilization techniques. Prehospital Emergency Care, 5(3), 270-274.
17. Ryan, D. W., Allen, V., & Murray, A. (1997). An investigation of interface pressures in low air loss beds. International Journal of Clinical Practice, 51(5), 296-298.
18. Defloor, T. (2000). The effect of position and mattress on interface pressure. Applied Nursing Research, 13(1), 2-11. doi:10.1016/S0897-1897(00)80013-0
19. Lovell, M. E., & Evans, J. H. (1994). A comparison of the spinal board and the vacuum stretcher, spinal stability and interface pressure. Injury, 25(3), 179-180. doi:10.1016/0020-1383(94)90158-9
20. United States Army Institute of Surgical Research. (2012). Joint theater trauma system clinical practice guideline: Spine injury surgical management and transport. Retrieved from http://www.usaisr.amedd.army.mil/assets/cpgs/Cervical_and_Thoracolumbar_Spine_Injury_9_Mar_12.pdf
21. Mok, J. M., Jackson, K. L., Fang, R., & Freedman, B. A. (2013). Effect of vacuum spine board immobilization on incidence of pressure ulcers during evacuation of military casualties from theater. Spine Journal, 13(12), 1801-1808. doi:10.1016/j.spinee.2013.05.028
About the author
Kenny Navarro is an Assistant Professor in the Emergency Medicine Education Department at the University of Texas Southwestern Medical Center at Dallas. He coordinates all continuing education activities and assists in medical oversight for BioTel, a multi-jurisdictional EMS system composed of 14 fire/rescue agencies and more than 1,500 paramedics. Mr. Navarro serves as a Content Consultant for the AHA ACLS Project Team for Guidelines 2010 and served on two education subcommittees for NIH-funded research projects, as the Coordinator for the National EMS Education Standards Project, and as an expert writer for the National EMS Education Standards Implementation Team. Send correspondence concerning any articles in this section to Kenneth W. Navarro, The University of Texas Southwestern Medical School at Dallas, 6300 Harry Hines Blvd, MC 9134, Dallas, Texas 75390-9134, or e-mailkenny.navarro@ems1.com.




No hay comentarios:
Publicar un comentario