VISITAS RECIENTES
We Support The Free Share of the Medical Information

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Enlaces PDF por Temas
- AHOGAMIENTO - ASFIXIA POR INMERSION - HIDROCUSION
- ALERTAS SANITARIAS MEDICAMENTOS Y EQUIPOS
- AMBULANCIAS
- Analgesia en EMS y TACMED
- ANATOMIA HUMANA
- ARMA BLANCA y Objetos Punzo-Cortates
- AUTISMO TEA Trastornos Espectro Autista TEA PDF
- BIOSEGURIDAD: Manuales y Guias PDF Gratis
- BUSQUEDA ONLINE DE MEDICOS EN IBEROAMERIA
- CODIGO INFARTO IAM: Todos los PDF Gratis
- BOMBEROS MANUALES PDF
- CAFÉ
- Control de Sangrados Torniquetes TQ STOP THE BLEED
- CORONAVIRUS covid-19
- CURSOS Medicos GRATIS /free online medical courses
- DENGUE todos los PDF Gratis
- DESASTRES: Guias y Manuales PDF Gratis
- Documentos 150 Aniversario ACADEMIA NACIONAL DE MEDICINA/ MEXICO
- ENFERMERIA
- EKG Libros PDF Gratis
- EMERGENCIAS OFTALMOLÓGICAS (oculares) OJOS
- FARMACOLOGIA PDF GRATIS
- GERIATRIA PDFs
- GUIAS CLINICAS PDF GRATIS MEXICO
- HISTORIA DE LA MEDICINA
- HURACANES ,TORMENTAS, CICLONES y TORNADOS
- ISRAEL
- ICTUS Todos los PDF Gratis
- LIBROS DE CIRUGIA EN PDF GRATIS
- MALARIA /Paludismo
- MEDEVAC / TACEVAC / CASEVAC / AROMEDICINA / TRANSPORTE AEROMEDICO
- MEDICINA MARITIMA todos los PDF
- MEDICINA todo lo relacionado a nuestra practica
- MEDICINA TACTICA: PDF Manuales y Guias
- OBESIDAD
- OBSTETRICIA y GINECOLOGIA PDF Gratis
- ocular oftalmologia
- El paquete técnico HEARTS by OMS/OPS
- Oxigenoterapia y Vias AEREAS
- OXIMETRIA todas las publicaciones
- PDFs Psicologia de Emergencias y DESASTRES
- PDF PICADURAS, MORDEDURAS, ARAÑAZOS, EMPONZOÑAMIENTOS
- Protocolos de Atencion Salud Dominicana
- Pediatria
- Perro-Canine-K-9-Firulais-Dugs-Chuchos-Canino
- QUEMADURAS
- RADIOLOGIA DIAGNOSTICO POR IMAGENES
- RCP Reanimacion CardioPulmonar PDF Gratis
- RIESGOS NIÑOS
- TELEMEDICINA
- TES Tecnico en Emergencias Sanitarias
- TRASTORNO ESPECTRO AUTISMO y URGENCIAS PDF
- TRIAJE PDF
- TRAUMA
- ULTIMOS post EMS Solutions Int
- EMS SOLUTIONS INTERNATIONAL
- IMPERIO ESPAÑOL
- PEDOFILIA: ¿COMO EVITAR ABUSO SEXUAL EN MENORES? INFOGRAFIA
- Perro / Vira Lata/ Canine/ K-9/ Firulais Dogs Chuchos/Canino todos los PDF
- REDES SOCIALES DRRAMONREYESMD
- SUBITUS INTERNATIONAL
- TORNIQUETE -TQ -Tourniquet
- Urologia
- VACUNAS
Nota Importante
Aunque pueda contener afirmaciones, datos o apuntes procedentes de instituciones o profesionales sanitarios, la información contenida en el blog EMS Solutions International está editada y elaborada por profesionales de la salud. Recomendamos al lector que cualquier duda relacionada con la salud sea consultada con un profesional del ámbito sanitario. by Dr. Ramon REYES, MD
Saturday, October 6, 2018
How to Master BVM Ventilation Bag mask ventilation / Free PDF Manual
 |
| How to Master BVM Ventilation Bag mask ventilation / Free PDF Manual |
Download FREE PDF Manual
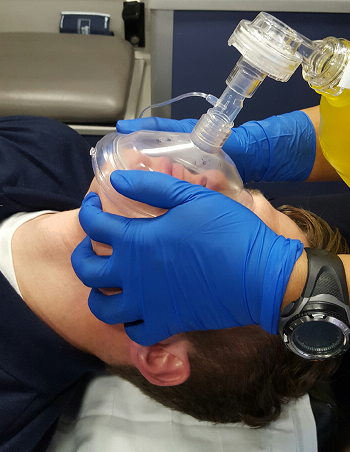
How to Master BVM Ventilation
Bag mask ventilation is the cornerstone of airway management.
It’s often considered a basic procedure, but there is nothing “basic” about BVM ventilation. Skill acquisition requires extensive training and experience. It’s not pretty, sexy, or glamorous. Most people perform it poorly even though it’s an essential part of good airway management.
We often relegate the skill to a new or junior provider, and when the saturation drops we attribute it to the patients’ acuity and not to failure to provide adequate oxygenation and ventilation.
The AHA recognizes that bag mask ventilation “is a challenging skill that requires considerable practice for competency.”
When performed in an emergency, respiratory failure or arrest is often imminent. Because it is a BLS skill we toss a BVM to our partner while we prepare our intubation equipment. The mask is placed on the patient’s face and ventilations are administered too aggressively or ineffectively.
When this is not recognized the airway may become flooded with gastric contents during the intubation attempt making more difficult if not impossible. Aspiration occurs, hypoxia worsens, and the patient is at higher risk of experiencing cardiac arrest.
It is not widely appreciated that BVM ventilation is often ineffective. One assumes that it works better than it actually does without appreciate education and training, which is often lacking.
Early in my career I would place the mask on the patient’s face and apply the CE technique without any objective measurement of how well it was working.
How do you Know When Ventilations are Effective?
Clinical detection of adequate ventilation is notoriously difficult. So what is the litmus test for gas exchange at the alveolar level? ETCO2 of course!
The ETCO2 sensor fits perfectly between the bag and mask.
In Emergency Medicine we want the technique that is most likely to be successful the first time. The traditional CE method is not always the best technique. Some will be quick to contest that assertion, and a few years ago I would have agreed with you.
Then I watched a video on EmCrit made by Reuben Strayer.
There are three main factors that contribute to poor BVM ventilation.
- Poor mask seal
- Improper positioning
- Excessive rate and volume
Poor Mask Seal
When using the traditional CE technique, pressure is not distributed equally across the mask. This means that when using your left hand, there is a tendency for air to leak between the mask and the right side of the patient’s mouth, which often goes unrecognized.
Improper Positioning
Because of the inherit difficulty maintaining a quality seal, and because maintaining a seal is fatiguing, the tendency is to push the mask onto the face. The mouth is then closed shut, leaving the nares as the only route of ventilation. Obstructive soft tissues of the pharynx collapse, blocking the glottic opening.
A superior technique was introduced 11 years ago in the 2005 AHA Guidelines.
“Bag-mask ventilation is most effective when provided by 2 trained and experienced rescuers. One rescuer opens the airway and seals the mask to the face while the other squeezes the bag. Both rescuers watch for visible chest rise.”
The two handed technique is sometimes referred to as the thenar eminence (TE), or “two thumbs down” technique.
The fingers are used to bring the jaw to the mask, while the palms and thumbs maintain a mask seal. This offers a mechanical advantage to the CE technique and allows better recognition of air leaks.
Gerstein (2013) compared the effectiveness of the CE and TE technique when performed by novice clinicians and found:
“The TE facemask ventilation grip results in improved ventilation over the EC grip in the hands of novice providers.”
A few weeks ago I attended a cadaver lab in Baltimore. The first skill we practiced was BVM ventilation. Our group leader has us try the CE technique first, then TE. The chest was open and lungs exposed so we could see the effectiveness of our ventilations.
Six people were in my group, and no one was able to inflate the lungs using the CE technique despite multiple attempts. However, the lungs were inflated every time, every attempt, for every person when using the TE technique!
Excessive Rate and Tidal Volume (Hyperventilation)
Even when trying to be cognizant of rate and tidal volume, there can be a huge difference in what you think you’re doing, and what you’re actually doing.
This was proven in the Milwaukee study, in which Paramedics were taught to ventilate at the appropriate rate during cardiac arrest. They retrospectively looked at the ventilation rates objectively and found the average rate was 30 breaths/min!
An excessive rate and tidal volume isn’t only deleterious for patients in cardiac arrest, but increases the likelihood of exceeding the pressure of the lower esophageal sphincter, delivering large tidal volumes of air to the stomach.
This also was mentioned back in the 2005 AHA Guidelines:
“Gastric inflation often develops when ventilation is provided without an advanced airway. It can cause regurgitation and aspiration, and by elevating the diaphragm, it can restrict lung movement and decrease respiratory compliance. Air delivered with each rescue breath can enter the stomach when pressure in the esophagus exceeds the lower esophageal sphincter opening pressure. Risk of gastric inflation is increased by high proximal airway pressure and the reduced opening pressure of the lower esophageal sphincter. High pressure can be created by a short inspiratory time, large tidal volume, high peak inspiratory pressure, incomplete airway opening, and decreased lung compliance.”
To prevent gastric inflation the airway must be kept open, and breaths delivered slowly…very slowly. Based on my observations no one delivers breaths slow enough. When your own heart rate is going 150 beats per minute, waiting 6 seconds to deliver a breath feels like forever! I often tell someone who is bagging to fast to deliver a breath every 10 seconds and even then they often ventilate too fast.
How do we slow down? Well, if the patient is intubated they could be placed on the ventilator. But since we’re talking about facemask ventilation, consider purchasing a timing light that goes on the end of the BVM, or use a metronome. You could also try counting, “one, one thousand…two, one thousand…three, one thousand…” and so on.
In addition to delivering breaths too fast, we deliver too much. The average volume of an adult BVM is 1600 milliliters! Squeezing the bag until opposite sides of the BVM touch isn’t necessary! It’s recommended that only 1/3 of the bag be compressed to give a large enough tidal volume. Any more and the pressure is too much for the rigid trachea to accommodate, and the esophagus is more than happy to accept the rest!
BVM Ventilation during Cardiac Arrest
If you’re doing 30:2 during BLS CPR you don’t have the luxury of providing breaths slowly. The goal should be to have compressions resumed within 3 seconds, and to do that the breaths can’t be given quickly or it will take 5 or 6 seconds!
The goal should be “little bag squeeze, little bag squeeze” with full release between squeezes. Intrathoracic pressure stays elevated without a full release, and we know that increased intrathoracic pressure impedes venous return.
Conclusion
- BVM ventilation is a difficult skill for providers at all levels and specialties.
- The traditional CE method is not very effective, and sometimes totally ineffective.
- Use ETCO2 as an objective measurement.
- Adopt the “two thumbs down” technique
- Deliver breaths slowly
- Only compress 1/3 of the bag
- Give breaths quickly during cardiac arrest, but allow full release of BVM
References“Beginner Facemask Ventilation Techniques | Emsworld.Com”. EMSWorld.com. N.p., 2016. Web. 17 Mar. 2016.
Gerstein NS, et al. “Efficacy Of Facemask Ventilation Techniques In Novice Providers. – Pubmed – NCBI”. Ncbi.nlm.nih.gov. N.p., 2016. Web. 17 Mar. 2016.
“Part 4: Adult Basic Life Support”. Circulation 112.24_suppl (2005): IV-19-IV-34. Web. 17 Mar. 2016
- See more at: https://www.aclsmedicaltraining.com/blog/master-bvm-ventilation/#sthash.BnI030nn.dpuf
Bag mask ventilation is the cornerstone of airway management.
It’s often considered a basic procedure, but there is nothing “basic” about BVM ventilation. Skill acquisition requires extensive training and experience. It’s not pretty, sexy, or glamorous. Most people perform it poorly even though it’s an essential part of good airway management.
We often relegate the skill to a new or junior provider, and when the saturation drops we attribute it to the patients’ acuity and not to failure to provide adequate oxygenation and ventilation.
The AHA recognizes that bag mask ventilation “is a challenging skill that requires considerable practice for competency.”
When performed in an emergency, respiratory failure or arrest is often imminent. Because it is a BLS skill we toss a BVM to our partner while we prepare our intubation equipment. The mask is placed on the patient’s face and ventilations are administered too aggressively or ineffectively.
When this is not recognized the airway may become flooded with gastric contents during the intubation attempt making more difficult if not impossible. Aspiration occurs, hypoxia worsens, and the patient is at higher risk of experiencing cardiac arrest.
It is not widely appreciated that BVM ventilation is often ineffective. One assumes that it works better than it actually does without appreciate education and training, which is often lacking.
Early in my career I would place the mask on the patient’s face and apply the CE technique without any objective measurement of how well it was working.
How do you Know When Ventilations are Effective?
Clinical detection of adequate ventilation is notoriously difficult. So what is the litmus test for gas exchange at the alveolar level? ETCO2 of course!
The ETCO2 sensor fits perfectly between the bag and mask.
In Emergency Medicine we want the technique that is most likely to be successful the first time. The traditional CE method is not always the best technique. Some will be quick to contest that assertion, and a few years ago I would have agreed with you.
Then I watched a video on EmCrit made by Reuben Strayer.
There are three main factors that contribute to poor BVM ventilation.
- Poor mask seal
- Improper positioning
- Excessive rate and volume
Poor Mask Seal
When using the traditional CE technique, pressure is not distributed equally across the mask. This means that when using your left hand, there is a tendency for air to leak between the mask and the right side of the patient’s mouth, which often goes unrecognized.
Improper Positioning
Because of the inherit difficulty maintaining a quality seal, and because maintaining a seal is fatiguing, the tendency is to push the mask onto the face. The mouth is then closed shut, leaving the nares as the only route of ventilation. Obstructive soft tissues of the pharynx collapse, blocking the glottic opening.
A superior technique was introduced 11 years ago in the 2005 AHA Guidelines.
“Bag-mask ventilation is most effective when provided by 2 trained and experienced rescuers. One rescuer opens the airway and seals the mask to the face while the other squeezes the bag. Both rescuers watch for visible chest rise.”
The two handed technique is sometimes referred to as the thenar eminence (TE), or “two thumbs down” technique.
The fingers are used to bring the jaw to the mask, while the palms and thumbs maintain a mask seal. This offers a mechanical advantage to the CE technique and allows better recognition of air leaks.
Gerstein (2013) compared the effectiveness of the CE and TE technique when performed by novice clinicians and found:
“The TE facemask ventilation grip results in improved ventilation over the EC grip in the hands of novice providers.”
A few weeks ago I attended a cadaver lab in Baltimore. The first skill we practiced was BVM ventilation. Our group leader has us try the CE technique first, then TE. The chest was open and lungs exposed so we could see the effectiveness of our ventilations.
Six people were in my group, and no one was able to inflate the lungs using the CE technique despite multiple attempts. However, the lungs were inflated every time, every attempt, for every person when using the TE technique!
Excessive Rate and Tidal Volume (Hyperventilation)
Even when trying to be cognizant of rate and tidal volume, there can be a huge difference in what you think you’re doing, and what you’re actually doing.
This was proven in the Milwaukee study, in which Paramedics were taught to ventilate at the appropriate rate during cardiac arrest. They retrospectively looked at the ventilation rates objectively and found the average rate was 30 breaths/min!
An excessive rate and tidal volume isn’t only deleterious for patients in cardiac arrest, but increases the likelihood of exceeding the pressure of the lower esophageal sphincter, delivering large tidal volumes of air to the stomach.
This also was mentioned back in the 2005 AHA Guidelines:
“Gastric inflation often develops when ventilation is provided without an advanced airway. It can cause regurgitation and aspiration, and by elevating the diaphragm, it can restrict lung movement and decrease respiratory compliance. Air delivered with each rescue breath can enter the stomach when pressure in the esophagus exceeds the lower esophageal sphincter opening pressure. Risk of gastric inflation is increased by high proximal airway pressure and the reduced opening pressure of the lower esophageal sphincter. High pressure can be created by a short inspiratory time, large tidal volume, high peak inspiratory pressure, incomplete airway opening, and decreased lung compliance.”
To prevent gastric inflation the airway must be kept open, and breaths delivered slowly…very slowly. Based on my observations no one delivers breaths slow enough. When your own heart rate is going 150 beats per minute, waiting 6 seconds to deliver a breath feels like forever! I often tell someone who is bagging to fast to deliver a breath every 10 seconds and even then they often ventilate too fast.
How do we slow down? Well, if the patient is intubated they could be placed on the ventilator. But since we’re talking about facemask ventilation, consider purchasing a timing light that goes on the end of the BVM, or use a metronome. You could also try counting, “one, one thousand…two, one thousand…three, one thousand…” and so on.
In addition to delivering breaths too fast, we deliver too much. The average volume of an adult BVM is 1600 milliliters! Squeezing the bag until opposite sides of the BVM touch isn’t necessary! It’s recommended that only 1/3 of the bag be compressed to give a large enough tidal volume. Any more and the pressure is too much for the rigid trachea to accommodate, and the esophagus is more than happy to accept the rest!
BVM Ventilation during Cardiac Arrest
If you’re doing 30:2 during BLS CPR you don’t have the luxury of providing breaths slowly. The goal should be to have compressions resumed within 3 seconds, and to do that the breaths can’t be given quickly or it will take 5 or 6 seconds!
The goal should be “little bag squeeze, little bag squeeze” with full release between squeezes. Intrathoracic pressure stays elevated without a full release, and we know that increased intrathoracic pressure impedes venous return.
Conclusion
- BVM ventilation is a difficult skill for providers at all levels and specialties.
- The traditional CE method is not very effective, and sometimes totally ineffective.
- Use ETCO2 as an objective measurement.
- Adopt the “two thumbs down” technique
- Deliver breaths slowly
- Only compress 1/3 of the bag
- Give breaths quickly during cardiac arrest, but allow full release of BVM
References“Beginner Facemask Ventilation Techniques | Emsworld.Com”. EMSWorld.com. N.p., 2016. Web. 17 Mar. 2016.
Gerstein NS, et al. “Efficacy Of Facemask Ventilation Techniques In Novice Providers. – Pubmed – NCBI”. Ncbi.nlm.nih.gov. N.p., 2016. Web. 17 Mar. 2016.
“Part 4: Adult Basic Life Support”. Circulation 112.24_suppl (2005): IV-19-IV-34. Web. 17 Mar. 2016
Gerstein NS, et al. “Efficacy Of Facemask Ventilation Techniques In Novice Providers. – Pubmed – NCBI”. Ncbi.nlm.nih.gov. N.p., 2016. Web. 17 Mar. 2016.
“Part 4: Adult Basic Life Support”. Circulation 112.24_suppl (2005): IV-19-IV-34. Web. 17 Mar. 2016
Vacuum Mattress Splint versus Long Backboard
 |
| Vacuum Mattress Splint versus Long Backboard |
Long Backboard versus Vacuum Mattress Splint to Immobilize Whole Spine in Trauma Victims in the Field: a Randomized Clinical Trial
by ketaminh on September 25, 2013
The Iranian authors claim this is the first RCT study of actual trauma patients , looking at performance of long hard backboard with vacuum mattress splint . IN their discussion they cite several past studies comparing the two methods of spinal immobilisation but note that these were only on healthy volunteers. They also state that as their RCT refutes all the findings of previous studies then further research to try to confirm their findings is warranted!
Surprisingly their findings claim that a hard backboard is SIGNIFICANTLY MORE COMFORTABLE than a vacuum mattress splint!
Not surprisingly, the vacuum mattress splint took longer to apply than the backboard.
The method to measure spinal immobilisation was also crude. Essentially an observer asked the patient to move their cervical and thoracolumbar spine in various directions and a guesstimate of the range of motion from VL ( very low) to VH ( Very high) was recorded ( 5 grades were used )
The major limitation of the study, indeed when comparing any medical device, is the familiarity with the users in the study. It was noted that the long backboard is the traditional method used in prehospital care in Iran. Lack of familiarity with actual prehospital use of the vacuum splint may have biased the recorded observations especially the time to apply as well as the immobilisation degrees measured.
The vacuum mattress splint in my view is more comfortable as its padded and holds the patient more securely in line. It definitely produces more of a sense of being cocooned in and this may elicit claustrophobic feelings in some patients. Perhaps this is the reason why patients rated the vacuum splint less comfortable? Also the unanswered question is how long were these transported patients on the backboard for? I suspect not long as we all know that the longer you spend on a hard surface the less comfortable it gets!
But kudos to our Iranian prehospital colleagues for trying to answer a question that is relevant to our PHARM community. Vacuum splints are expensive and break easily so it is no mean cost to have and use them.
Information from prehospitalmed.com
The method to measure spinal immobilisation was also crude. Essentially an observer asked the patient to move their cervical and thoracolumbar spine in various directions and a guesstimate of the range of motion from VL ( very low) to VH ( Very high) was recorded ( 5 grades were used )
 |
| Vacuum Mattress Splint versus Long Backboard |
Prehosp Disaster Med. 2013 Oct;28(5):462-5. doi: 10.1017/S1049023X13008637. Epub 2013 Jun 10.
Long backboard versus vacuum mattress splint to immobilize whole spine in trauma victims in the field: a randomized clinical trial.
Author information
Abstract
INTRODUCTION:
Patients with possible spinal injury must be immobilized properly during transport to medical facilities. The aim of this research was comparing spinal immobilization using a long backboard (LBB) with using a vacuum mattress splint (VMS) in trauma victims transported by an Emergency Medical Services (EMS) system.
METHODS:
In this randomized clinical trial, 60 trauma victims with possible spinal trauma were divided to two groups, each group immobilized with one of the two instruments. Speed and ease of application, immobilization rate, and the patients' comfort were recorded.
RESULTS:
In this survey, LBB was faster to apply: 211.66 (SD = 28.53) seconds vs 654.00 (SD = 16.61) seconds. Various measures of immobilization were better by LBB. Also, LBB offered a significant improvement in comfort over a VMS for the patient with possible spinal injury. All of the results were statistically significant.
CONCLUSION:
The results of this study showed that immobilization using LBB was easier, faster, and more comfortable for the patient, and provided additional decrease in spinal movement when compared with a VMS.
Comment in
- Author reply: To PMID 23746392. [Prehosp Disaster Med. 2014]
- The Long Backboard vs the Vacuum Mattress. [Prehosp Disaster Med. 2014]
- PMID:
- 23746392
- [PubMed - indexed for MEDLINE] http://www.ncbi.nlm.nih.gov/pubmed/23746392
- Author reply: To PMID 23746392. [Prehosp Disaster Med. 2014]
- The Long Backboard vs the Vacuum Mattress. [Prehosp Disaster Med. 2014]
- PMID:
- 23746392
- [PubMed - indexed for MEDLINE] http://www.ncbi.nlm.nih.gov/pubmed/23746392
Original Research
Long Backboard versus Vacuum Mattress Splint to Immobilize Whole Spine in Trauma Victims in the Field: a Randomized Clinical Trial
Babak Mahshidfara1, Mani Mofidia1 c1, Ali-Reza Yaria1 and Saied Mehrsorosha2
a1 Tehran University of Medical Sciences, Tehran, Islamic Republic of Iran
a2 Tehran Emergency Medical Service System, Tehran, Islamic Republic of Iran
Abstract
Introduction Patients with possible spinal injury must be immobilized properly during transport to medical facilities. The aim of this research was comparing spinal immobilization using a long backboard (LBB) with using a vacuum mattress splint (VMS) in trauma victims transported by an Emergency Medical Services (EMS) system.
Methods In this randomized clinical trial, 60 trauma victims with possible spinal trauma were divided to two groups, each group immobilized with one of the two instruments. Speed and ease of application, immobilization rate, and the patients’ comfort were recorded.
Results In this survey, LBB was faster to apply: 211.66 (SD = 28.53) seconds vs 654.00 (SD = 16.61) seconds. Various measures of immobilization were better by LBB. Also, LBB offered a significant improvement in comfort over a VMS for the patient with possible spinal injury. All of the results were statistically significant.
Conclusion The results of this study showed that immobilization using LBB was easier, faster, and more comfortable for the patient, and provided additional decrease in spinal movement when compared with a VMS.
B Mahshidfar, M Mofidi, A Yari, S Mehrsorosh. Long backboard versus vacuum mattress splint to immobilize whole spine in trauma victims in the field: a randomized clinical trial. Prehosp Disaster Med. 2013;28(5):1-4 .
(Received July 29 2012)
(Revised November 24 2012)
(Accepted December 02 2012)
(Online publication June 10 2013)
Keywords
- immobilization;
- long backboard;
- prehospital;
- trauma;
- vacuum mattress splint
Abbreviations
- EMS:Emergency Medical Services;
- LBB:long backboard;
- VMS:vacuum mattress splint
Correspondence
c1 Correspondence: Mani Mofidi, MD Tehran University of Medical Sciences Rasoul Akram Hospital, Emergency Department Sattarkhan Ave, Nyaiesh St. Tehran, Islamic Republic of Iran E-mail m-mofidi@sina.tums.ac.ir
Footnotes
Conflicts of Interest: None.
http://journals.cambridge.org/action/displayAbstract;jsessionid=BCEF11F96C0358D8F329416C0658D559.journals?aid=9030584&fileId=S1049023X13008637
 |
| Dr. Ramon REYES DIAZ, MD |
Montañas "Medidas de prevención"
 |
| Montañas "Medidas de prevención" |
- Montañas "Medidas de prevención"
- Siempre que salga a la montaña, deje dicho dónde va. Nunca vaya solo.
- Infórmese antes de salir de la predicción meteorológica y del riesgo de aludes.
- El material y equipo que vaya a utilizar deberán estar siempre en perfectas condiciones de uso.
- Guarde fuerzas para el regreso. Si es preciso, hay que saber renunciar.
- Utilice mapas y libros. Si carece de experiencia, acuda a los guías de montaña.
- Realice cursos de primeros auxilios en montaña. Le enseñarán a prevenir y actuar en caso de accidente.
- Cuide su preparación física. El montañismo exige estar en buena forma.
- En caso de que disminuya la visibilidad por niebla, no siga caminando, permanezca quieto en un lugar fijo y seguro hasta que aquélla desaparezca.
Medidas de autoprotección en caso de accidente
- Avise lo antes posible a los medios de socorro (112). Si no tiene teléfono, piense en el refugio o pueblo más cercano y la forma de llegar a él.
- Si está con un herido y es posible, no lo deje solo.
- Al informar sobre el accidente, es importante especificar con claridad: lugar exacto donde se encuentra la víctima y características del terreno, accesibilidad, condiciones meteorológicas en el lugar, estado del accidentado.
LOS TRAUMAS INFANTILES CAMBIAN EL CEREBRO Y PREDISPONEN A LA VIOLENCIA
 |
| LOS TRAUMAS INFANTILES CAMBIAN EL CEREBRO Y PREDISPONEN A LA VIOLENCIA |
Un estudio de la EPFL demuestra por vez primera una relación entre el sufrimiento psicológico temprano y el comportamiento agresivo.
Un equipo de investigadores de la Escuela Politécnica Federal de Lausana (EPFL) de Suiza ha demostrado por primera vez la existencia de una correlación entre el trauma psicológico y cambios concretos y perdurables en el cerebro, unos cambios que, además, estarían vinculados con el comportamiento agresivo. Los científicos analizarán ahora si tratamientos específicos podrían revertir esta transformación del cerebro, gracias a su plasticidad.
Es bien sabido que muchos individuos violentos han sufrido traumas psicológicos durante la infancia. Algunas de estas personas también presentan alteraciones en la corteza orbitofrontal (COF). Pero, ¿existe una relación entre estos cambios físicos en el cerebro y una infancia psicológicamente traumática? ¿Pueden las experiencias modificar la estructura física del cerebro?
Un equipo de investigadores de la Escuela Politécnica Federal de Lausana (EPFL), dirigido por la profesora Carmen Sandi, miembro de los Centros Nacionales SYNAPSY, ha demostrado por primera vez una correlación entre el trauma psicológico y cambios concretos en el cerebro, a su vez vinculados con el comportamiento agresivo.
En ratas, la experiencia de un trauma pre-adolescente produce un comportamiento agresivo acompañado por cambios estructurales y funcionales del cerebro, los mismos observados en seres humanos violentos. En otras palabras, las heridas psicológicas sufridas en la infancia dejan una huella biológica duradera, que persiste en el cerebro adulto. Los resultados de esta investigación han aparecido publicados en el número de enero de la revista Translational Psychiatry.
“Esta investigación demuestra que las personas expuestas a un trauma en la niñez no sólo sufren psicológicamente, sino que además padecen alteraciones cerebrales”
Explica Sandi directora del Laboratorio EPFL de Genética del Comportamiento y directora del Instituto Brain Mind.
“Esto añade una dimensión adicional a las consecuencias del abuso, y obviamente tiene implicaciones científicas, terapéuticas y sociales”
Añade la investigadora en un comunicado de la EPFL. Los investigadores consiguieron desentrañar las bases biológicas de la violencia estudiando a un grupo de ratas macho, que fueron expuestas a situaciones psicológicamente estresantes durante su juventud. Después de observar que estas experiencias llevaron a las ratas a un comportamiento agresivo en la edad adulta, los científicos examinaron lo que ocurría en el cerebro de estos animales, con el fin de determinar si el período traumático había dejado o no una huella duradera.
“En una situación social difícil, la corteza orbitofrontal de un individuo sano se activa, con el fin de inhibir los impulsos agresivos y de mantener una interacción normal”, explica Sandi.
“Pero en las ratas que estudiamos, nos dimos cuenta de que había muy poca activación de la corteza orbitofrontal. Esto, a su vez, redujo su capacidad para moderar sus impulsos negativos. Además, esta reducción de la activación vino acompañada por la sobreactivación de la amígdala, una región del cerebro que está implicada en las reacciones emocionales”.
“Otros investigadores especializados en el estudio del cerebro de los humanos violentos ya habían observado el mismo déficit en la activación orbitofrontal, así como la misma y simultánea inhibición reducida de los impulsos agresivos. Es asombroso; no esperábamos encontrar estos niveles de similitud”, afirma Sandi.
Los antidepresivos y la plasticidad cerebral
Los científicos también midieron los cambios en la expresión de ciertos genes en el cerebro. Se centraron en los genes que se sabe están involucrados en comportamientos agresivos, para los que existen polimorfismos (variantes genéticas) que predisponen a sus portadores a una actitud agresiva. Se analizó si el estrés psicológico experimentado por las ratas causaba una modificación en la expresión de estos genes.
“Hemos descubierto que el nivel de expresión del gen MAOA aumentó en la corteza prefrontal”, explica la investigadora. Esta alteración fue vinculada a un cambio epigenético; en otras palabras, la experiencia traumática terminó provocando una modificación a largo plazo de la expresión de este gen.
Finalmente, los investigadores trataron de ver si un inhibidor del gen MAOA, en este caso un antidepresivo, podía revertir el aumento en el comportamiento agresivo de las ratas, inducido por el estrés juvenil. El tratamiento fue eficaz.
El equipo concentrará ahora sus esfuerzos en tratar de entender mejor estos mecanismos, en explorar si existe un tratamiento que pudiera revertir estos cambios en el cerebro y, sobre todo, en tratar de arrojar luz sobre el efecto de la composición genética en la vulnerabilidad hacia el desarrollo de la agresividad.
Por otra parte, “esta investigación también podría revelar la capacidad de los antidepresivos de renovar la plasticidad cerebral”, concluye Sandi.
Descodificación Biológica de Enfermedades.
Edgar Mendizabal
Especialista en Descodificación Biológica.
Acompañante en BioNeuroEmoción.
Conferencista en Psicosomática Clínica
Consultas al: 5544523905
memoriaemocional.com
Referencia bibliográfica:
C Márquez, G L Poirier, M I Cordero, M H Larsen, A Groner, J Marquis, P J Magistretti, D Trono, C Sandi. Peripuberty stress leads to abnormal aggression, altered amygdala and orbitofrontal reactivity and increased prefrontal MAOA gene expression. Translational Psychiatry (2013). DOI: 10.1038/tp.2012.144.
Subscribe to:
Posts (Atom)