 |
| Dr. Ramon Reyes Diaz, MD CPR practice at the EMSWORLD Expo 2010 Dallas, Texas. USA |
By Forrest Winslow
Surviving a Cardiac Arrest is NOT "Automatic"; its Manual! Is a bit of play on words. There are many steps a healthcare provider can take to increase the likelihood of a patient surviving a Sudden Cardiac Arrest (SCA). The first is decrease the time off the chest around delivering a defibrillation. The time is referred to as peri-shock pause and the most efficient way to make this happen is to operate the defibrillator in "manual" mode. The human eye can recognize VF (Ventricular Fibrillation) in less than a second and if the monitor is pre-charged, we can quickly deliver the shock and go back to compression with minimal interruptions.
In almost all cases, it's best to stay on the scene to work a cardiac arrest resuscitation until the return of spontaneous circulation or efforts are stopped due to futility, according to Dr. Brent Myers, medical director of Wake County EMS System in Raleigh, N.C.
Patients with an increased time off of the chest around the defibrillation are far less likely to survive their SCA neurologically intact. [1] So make it manual if it's in your scope of practice.
Data has proven your chances of surviving a sudden cardiac arrest is 11x more likely if you live in one county/city vs. another. 55% versus 5%.
Stop Moving & Do Compressions! So often in the past we were taught definitive care was in an emergency department, as pre-hospital providers we shot for that goal and quickly moved the patient while attempting an ongoing resuscitation. How foolish is that logic. It is a rare case when the hospital can do more than EMS to correct a pulseless state. The key to have a patient survive neurologically intact is high quality CPR and every moment we put to packaging and moving we are not focused on high quality compressions and meeting critical benchmarks of resuscitation.
We absolutely need to attempt an active resuscitation where the patient presents in cardiac arrest, even if this is the ambulance bay of the emergency department. Every second counts, so make them count and do what is right. Furthermore because of the sheer number of cardiac arrest we manage we are far better at resuscitation than our hospital partners and we need to own this part of our patients care. To quote Dr. Brent Myers "resuscitation is a prehospital enterprise, post resuscitation care is a hospital enterprise".
Light them up every 2 minutes without interruption & switch compressors! It is important to stay on a cycle of checking pulses every 2 minutes and precharge the monitor prior to pause for a rhythm and pulse check. Our goal is to limit breaks in CPR to 10 second or less. By pre-charging the defibrillator we are less likely to have big breaks in CPR.
Changing compressors every 2 minutes has proven to increase the quality of CPR. Even a very healthy provider decreases by some degree after 2 minutes of compressions, especially when they focus on active recoil and not resting on the chest between compressions.
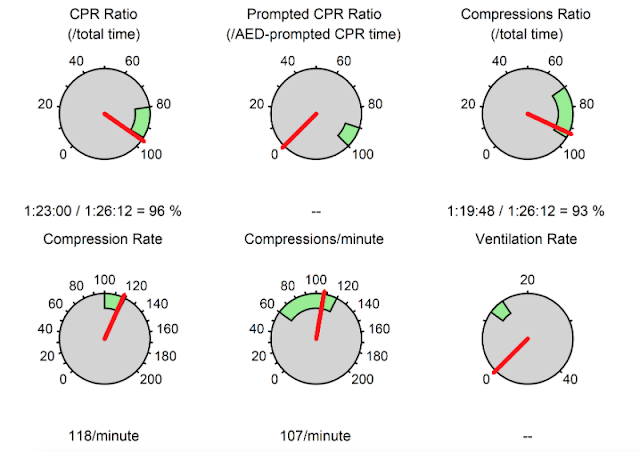
CPR analytics will open your eyes! If your service has tools or software that will provide feedback on the quality of you CPR, use it. I recently reviewed a cardiac arrest and the crew was sitting right at 50% compression ratio and their rates were 90-160/minute. After reviewing the data with the crew they orchestrated a resuscitation a few days later that was nearly flawless and with a 96% CPR ratio. They also decreased their peri-shock pauses by 30 seconds on average.
Measure ETCO2 to guide ROSC & TORP! End-tidal carbon dioxide monitoring is a must in any critically ill patient, especially ones experiencing a cardiac arrest. ETCO2 initially was used to confirm and monitor endotracheal tube placement. Over the last decade EMS has expanded its use and it has
become a valuable tool to guide our care in resuscitation. It should be placed on the patient as soon as possible even when maintaining a BLS airway. It can provide instant information about perfusion status, quality of compressions, Return of Spontaneous Circulation (ROSC), and even guide our decisions about Termination of Resuscitation Processes (TORP).
Santa Checks his list twice and so should you! For years the aviation industry has used the checklist to ensure critical steps are not missed. If list are good for pilots and Santa they are definitely good for healthcare providers that are making life or death decisions under very stressful situations. A checklist should not be a protocol in list form but a list of critical task that make a clear difference in patient's outcomes. At a minimum we should have one for an active resuscitation; post ROSC & TORP.
Data has proven your chances of surviving a sudden cardiac arrest is 11x more likely if you live in one county/city vs. another. 55% vs. 5%. There are many factors that go into making a system that fully embraces all the links in the "Chain of Survival" but I suggest we start with the low hanging fruit and do the things that are within our control and financial resources. The final thing is to make yourself a Resuscitation Champion for your system. By simply being aware of best practices, providers can adjust and improve things within their scope of practice. After you tighten up your game then profess the evidence to your leaders and fellow providers to drive the rest of the system.
https://www.linkedin.com/pulse/surviving-sudden-cardiac-arrest-automatic-its-manual-forrest-winslow
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2661879/
 |
| TELEFUNKEN AED DESFIBRILADOR FULL AUTOMATICO |
TELEFUNKEN AED DESFIBRILADOR FULL AUTOMATICO "0" RIESGOS
DISPONIBLE EN AMERICA (REPUBLICA DOMINICANA)
Contactos:
+1 849 865 4142 Rep. Dominicana
+34 640 220 306 (Numero Internacional en España)
eeiispain@gmail.com
Skype: drtolete
Facebook: @drramonreyesdiaz
LinkeIn https://es.linkedin.com/in/drramonreyes
Twitter: @DrtoleteMD
I nstagram: https://www.instagram.com/drtolete/
DISPONIBLE EN AMERICA (REPUBLICA DOMINICANA)
Contactos:
+1 849 865 4142 Rep. Dominicana
+34 640 220 306 (Numero Internacional en España)
eeiispain@gmail.com
Skype: drtolete
Facebook: @drramonreyesdiaz
LinkeIn https://es.linkedin.com/in/drramonreyes
Twitter: @DrtoleteMD
I nstagram: https://www.instagram.com/drtolete/





No hay comentarios:
Publicar un comentario